Roux-en-Y Gastric Bypass (RYGB) Leak and Management
Leaks are uncommon in RYGB. Around 1/100 cases will develop a leak in primary bypass. If you have had a band or stapling procedure, this figure is 1/50. Leaks often present late. This means at around the 2 week point. They are usually due to poor blood supply to the top of the stomach. It is usually not possible to determine this at the time of surgery. Eating in the first 2 weeks is also a big risk and that is why we use a liquid only diet for 2 weeks. Other risk factors for leaks are diabetes and smoking.
RYGB is the best option for poorly controlled diabetics. A recent long term study called the STAMPEDE trial, showed a 50 % remission rate at 5 years. Meaning that 5 years after the RYGB, the patients were still no longer on medications and had a normal HbA1c (a marker of diabetic control).
Leaks are usually treated with the gastroscope and rarely require another major operation. Always ring Border Surgical before anyone wants to operate on you and make sure they are aware of the operation you have had.
The CT scan above shows an 8 cm mixed fluid and gas filled abscess. This patient is 55 year old man with Type II Diabetes. He was on daily Insulin but is otherwise well. He has a BMI of 35 (weight 100kg) and has had no previous surgery/bariatric surgery. I performed a standard Gastric Bypass and he was discharged 3 days after surgery on fluids. 16 days post operatively he developed a fever, mild left side chest pain, some nausea and struggling to move to sloppy phase of diet.
The patient underwent a gastroscopy and the fluid and gas were drained. A .5 cm hole was seen and a small drain was placed via the gastroscope and left for 6 weeks. This was then removed with complete resolution of the collection and leak.
At 3 months he has now lost 20 kgs and is no longer on Insulin.
Sleeve Gastrectomy leak
Sleeve leaks are feared by all. They are hard to treat because the hole is kept open by the pressure in a narrow sleeve. Bougie size is important in minimising the chance of leak and their ability to seal off. I use a 40 French bougie. Studies have shown bougie size less than 32 French is statistically more likely to leak. The tightness of the sleeve doesn’t mean more weight loss. Studies show the same weight loss at 3 years with 32 French vs 40 French. The difference is in reflux and leaks which are higher in tighter sleeves.
It is important you don’t smoke or eat in the first 2 weeks.
Most of these leaks are due to blood supply. Other causes are eating too early and a very tight sleeve. They are almost always from the very top of the sleeve which is the area with the most dubious blood supply. Treatment of these is almost always with the gastroscope. Generally, we will give the sleeve a stretch with a balloon and then place a drain in the hole.
Never let anyone operate on you without discussion with me. Even if its 2 am! Surgery is rarely needed and can make things a lot worse.
The above CT scan shows a liquid and gas filled collection at the top of the sleeve. This patient is a 43 year old man. He presented with a BMI 36. I performed a standard Sleeve Gastrectomy with a 40 french Bougie. No leaks were shown when we performed a test in theatre with blue dye. Normal post operative blood tests were performed.
2 weeks post his Sleeve procedure he had nausea and a fever, felt generally unwell and had left shoulder tip pain. We performed an immediate gastroscopy and found a .5 cm defect or hole and drained the fluid and air. A drain was then placed in the hole and left for 6 weeks. He was allowed immediate fluids and discharged in 2 days. The drain was removed in 4 weeks with complete resolution of the leak.
The Perfect Band
A perfect band is one that gives just enough restriction that a small meal will make you feel full. I am of the firm belief that you need no more than 4-5 mls in a standard small lap band. Anymore than this will eventually cause esophageal dilatation or stretching of the esophagus above the band.
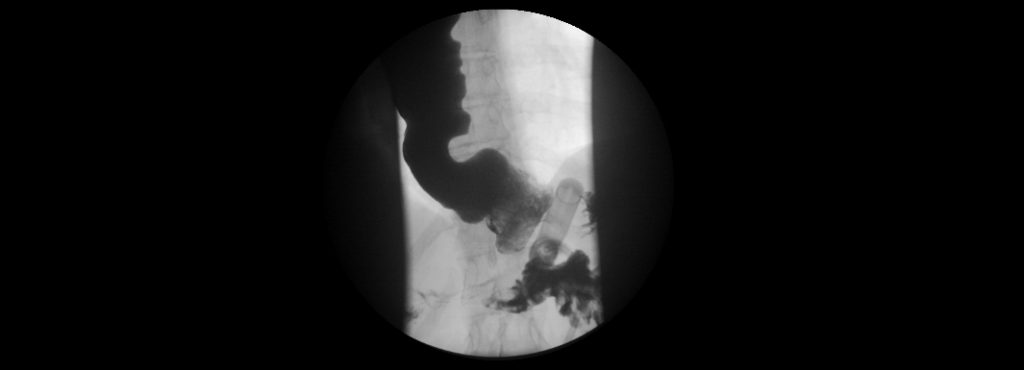
Below is a photo of a barium showing a perfect band. Note the band position is 2 to 7 o’clock and there is a small pouch above the band. A Barium swallow mixed with bread or marshmallow gives the most information about position of the band and state of the esophagus. It also allows the radiologist to see how well the esophagus empties through the band. All-important pieces of the puzzle.
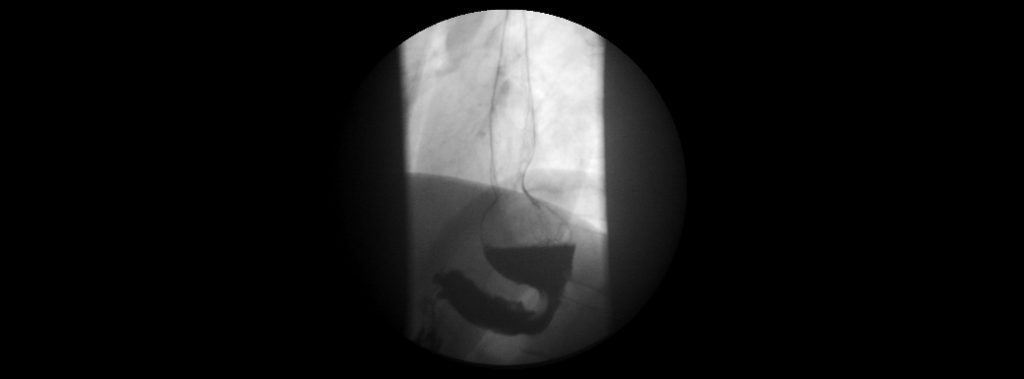
Compare this band with the one below. The band below is in a reasonable position but there is gross esophageal dilatation from putting too much fluid in it. When I took the fluid out there was 11 mls in it. Unfortunately she required removal of the band and a gastric bypass. She has done very well.
The real issue with esophageal dilatation is that it is almost impossible to get the feeling of restriction you had in the beginning. My experience is that the band is now going to be ineffective for further weight loss and unless you can adjust your lifestyle and diet to aid weight loss, you are likely best to consider some type of revisional surgery. This is often very disappointing for most people and is the reason I am so strict with adjustment of the band. Dilatation above obstruction is a normal response or adaptation of the body to obstruction. This is why relying on obstruction or restriction with a gastric band is only a short term fix.
The Over Adjusted Gastric Band
A number of patients present to me with failure to lose weight and the first thing they ask is for their band to be adjusted. They feel that more fluid in their band will result in more weight loss. I have a number of patients who have an expectation that more fluid equals weight loss and unfortunately, I have to tell them that this is not the case.
The band is designed to work by restriction not obstruction. There is a subtle difference between these two features. With obstruction, it is almost impossible to eat any solid food and in particular, the solid food I want them to eat is high protein solid food. What you do then is you tend to develop a propensity to eat high carbohydrate food. This sort of food will go through an obstructed band as it is often liquid when it hits the band. This results in what I call maladaptive eating behaviour. The end result of this is that you will put on weight rather than lose weight. The other problem is that you risk complications of the band such as gastric band prolapse or slip and also damage to the lower oesophagus through reflux. The other thing that I often see with patients that have too much fluid in their band is a dilated esophagus. This means that you are actually developing a second stomach above the band, which can hold increased amounts of food.
A dilated esophagus usually settles but may be permanent. A Barium swallow is useful in determining this.
The perfect band allows you to be able to eat solid food including meat and chicken. If you can eat these foods you will feel full. It is also high in protein and this does not get converted into fat. Although we do not want people eating too much, we want them to be able to have a good range and variety of food. Sometimes the best solution for people who are not losing weight, or putting on weight, is to take fluid out of their band so that they can go back to eating good quality food. This surprises some people as they naturally think that this will cause weight gain. I am happy to discuss this with you at your next consultation or adjustment.
Gastric Band Slip
This 36-year-old lady had a gastric band inserted 5 years ago. It had been adjusted to 7 mls of fluid. She had been struggling for a few weeks with solid food and had recently developed heartburn and reflux symptoms at night. She commented that she had not had a full night’s sleep for weeks. Her weight loss was good losing 22 kg. Her BMI now was 31.
Another Slip
A 39 year old lady presented with reflux at night and extreme weight loss due to inability to eat solids at all. The following barium was obtained.
My Comment:
These 2 cases are classic of a gradual or non acute slip. Over time, the stomach under the band has moved above the band causing a large pouch that empties poorly. This means food tends to stay in the pouch for a long time and often is regurgitated into the esophagus or mouth. Heartburn and reflux especially at night is a classic symptom and cannot be ignored. Weight loss will often stagnate and often weight will increase with a chronic slip because people tend to rely on calories from high calorie liquids. This is call maladaptive eating behavior.
Solution:
This needs an operation. There is no means to solve this without some sort of revisional surgery. Firstly though, the band needs to be emptied and a barium swallow done to confirm the diagnosis. We can then talk through some sort of revision. This may be another band or removal and revision to sleeve or bypass. Everybody is different and this decision is one that is made carefully. I don’t like to re band at the time of removal, this is difficult and may lead to poor outcomes in the future.
A special comment on reflux and bands
If you have a band and begin to experience any heartburn or reflux then you need to seek advice. Bands are actually an anti reflux valve if sitting correctly. Reflux indicates either a structural problem with the band or esophageal dilatation. It is best to see your surgeon in this case.
Esophageal Dilatation
This 47 year old man presented with weight gain and ability to eat a lot more food than he previously could. This occurred over a period of 6-12 months. He had his last adjustment 1 year ago and wasn’t sure of the amount in his band. When pushed he was vomiting food and had occasional reflux.
My Comment:
This is a classic case of esophageal dilatation. This is a result of chronic or long term obstruction of the esophagus. The esophagus is a hollow muscular tube that is designed to move food from the mouth to stomach. It does this via coordinated contractions of the muscle. If the esophagus is partially blocked then the body will respond by widening or dilating to cope with the hold up at the level of the band. The esophagus eventually loses its tone and dilates like a balloon. This results in the ability to tolerate more food and often lose the restriction that band patients crave. Essentially, the esophagus acts as a stomach above the stomach. The food will eventually fall through the band but even the slightest adjustment can tip the patient over the edge and result in vomiting and regurgitation. This is a serious problem. Often the patient has a lot of fluid in the band. I have seen as much as 13 mls in a 10 ml band!
Solution:
This is a difficult problem. There is not a lot of data or a general consensus for management. It is currently a subject of my own research. My experience is that once the esophagus dilates to the extent of the above x-ray, it is almost impossible to get sustained weight loss without some sort of revision. My first approach is to release the band to 3 mls and wait for 6 weeks. We then repeat the barium. Often the esophagus has returned to normal size. In this time it is important to get some advice from our dietitian’s. The real problem is that re adjustment is often unsatisfactory and we just end up in the same situation.
Revision for this sort of patient would have to be conversion to RYGB. A sleeve will not work as the patient will have an esophagus bigger than the sleeve and will lack restriction. Sometimes a minimizer ring can be used with the sleeve, but this is not proven. This problem requires discussion between surgeon and patient with pros and cons clearly outlined.
Another case
Similar to the previous case, this lady has gross esophageal dilatation. She presented with aspiration pneumonia. This is essentially inhaling one’s own vomit. She had a full band with 10 mls of fluid.
I have performed a Roux-en-Y Gastric Bypass on her and she has recovered very well. I removed the band at the same time as she had previous surgery, which meant keyhole surgery was not possible.
Pouch Dilatation
This 57 year old man presented with reflux and difficulty adjusting the band. Every time we added even a small amount of fluid he would obstruct or block. He was also eating high calorie liquids and sloppy food which was resulting in weight re gain. He had gained 7 kg in 4 weeks. The reflux was terrible and he was placed on an antacid drug called Nexium.
Discussion:
This barium study shows a pouch above the band. This is probably related to high pressures generated above the band. There is likely a hiatal hernia also associated with this. My solutions for this is to remove the fluid and re educate the patient. The problem is the pouch will not resolve itself and will often need surgical revision. This will often involve a hiatal hernia repair. In this case I removed the band and waited 3 months to revise. I have since converted him to a RYGB. This was done using keyhole surgery and he only spent 3 days in hospital.
Band Erosion
This condition is not common.
This 47 year old man presented with failure to lose weight. He currently weighs 184 kgs. He also suffered from pain at the port site and vague left abdominal pain after food.
An erosion is where the band gradually cuts through into the stomach. It is often associated with port infections. Infection spreads from the stomach to the tubing and then the port.
This man will need the band removed. I will do this via the gastroscope. Sometimes this is not possible and needs a laparoscopic approach.
I would only recommend revision after a minimum of 3 months. I would also only recommend RYGB as the operation for revision.
Band to sleeve after erosion
This lady was referred after a revisional sleeve gastrectomy was performed after an eroded band. There is a large pouch above the bulk of the sleeve. This lady had a lot of trouble with reflux and starting solid food after her sleeve.
I performed a gastroscopy and gently dilated the sleeve beyond the pouch and things have improved. I would recommend that if you have an eroded band, the best way forward is a RYGB. The other issue here is that the pouch was likely present before the sleeve. As the sleeve has very high pressures in the stomach, a pouch will not empty well. Reflux and vomiting can then occur. A pouch is a relative indication for a RYGB. More importantly, an eroded band is high risk to revise and you should always wait at least 3 months before revision surgery.
Previous Stapling
I see quite a few patients with previous gastric stapling. In Melbourne, this was almost always a High Gastric Reduction (HGR). These involved creation of a small upper stomach pouch with a row of staples that can’t be removed. The pouch was kept closed by 2 or 3 non-absorbable sutures. This operation often failed because people stretched the pouch or they had a breakdown in the staple line.
These operations can only be revised to a RYGB. Putting a band above a stapling is a bad operation in my opinion for a variety of reasons.
This revision is complex and often done by open surgery. It requires not only RYGB but often excision of the staple line. This is called fundectomy. I am happy to discuss this procedure further with you at your next consultation.
To Sleeve or not to Sleeve?
This case study shows a lady who had 2 previous gastric bands. Although she had lost substantial weight she was eating more than she should. Her barium study showed a dilated esophagus and tight band. We took the band out and performed aSleeve Gastrectomy. Unfortunately she could not tolerate liquids post op. The barium done post sleeve showed a tight blockage at the level of the previous band. This was very badly scarred from the band. We placed a stent through the area for 6 weeks and she improved dramatically.
Although the esophagus is still dilated the sleeve is now not obstructed. This is an excellent result but ultimately a RYGB may have been a better option both in the short term and in the long term given the degree of esophageal dilatation.
In general, I am not enthused about Band to Sleeve. I think it’s difficult to predict who will do well and who will get complications.
The Tight Sleeve
A 30 year old lady presented with morbid obesity. Her weight was 120 kg when she presented to me and her BMI was approximately 38. She was a large volume eater and had a propensity towards eating high carbohydrate food. We discussed options available to her and decided on a Sleeve Gastrectomy. She underwent a Sleeve Gastrectomy successfully. Over the next 18 months she lost significant amounts of weight and got down to 65 kg. She did this by modifying her diet and also exercising extensively. Unfortunately, she developed reflux and left upper quadrant pain. Her reflux was most of the time and had substantially affected the amount of food she could eat and the quality of the food.
We performed a barium swallow and you can see a dilated part of the sleeve above an area we call the incisura. This causes a blockage of this area because it is a very narrow part of the stomach. This resulted in stretching of the top part of the sleeve, which was holding food and causing reflux into the lower oesophagus or gullet.
This is an unusual complication of Sleeve Gastrectomy, however, one that does require a surgical solution. We then performed a re-sleeve of the stretched part of the sleeve and then a Roux-en-Y gastric bypass. She is now two months postoperative and has lost a further 5 kg and feels great.
This is a rare complication following Sleeve Gastrectomy. The most common cause is the natural narrowing we see in the part of the stomach that we call the incisura. In performing the sleeve, we try and stay well wide of this point but even when we do this, it is sometimes not enough to stop the blockage. Conversion of the sleeve to Roux-en-Y gastric bypass usually gives a successful outcome and most patients are immediately satisfied with the result.
Reflux after RYGB
This is very unusual and you should always seek advice from your surgeon.
I initially performed a primary sleeve on this 62 year old man. He presented with a BMI of 45 and diabetes requiring insulin. He initially lost 28 kg after the sleeve and was able to stop all insulin. Unfortunately he developed reflux and on Barium there was a stenosis or tightening of the sleeve. I then converted him to RYGB. Unfortunately, after 3 years he regained weight and was back on insulin with major food intolerance and reflux.
I performed a gastroscopy and found a redundant jejunal part of his join between gastric pouch and stomach. There was also functional blockage of the join with bowel prolapsing through the join.
I re operated and removed the excess bowel. I then re did the join and placed a minimizer ring to prevent dilatation of the join. I also lengthened his bypass limb, which was only 1 metre long. I lengthened it to 1.5 metres.
This was done by open surgery. Amazingly, weight loss has restarted and he has stopped all diabetic medications. Below is the finished join and the minimizer ring above the join.
Comments:
In rare instances, Sleeve conversion to RYGB for reflux or obstruction is required. We are very careful to leave a lot of room at the bottom of the sleeve and not narrow it. In this case the patient had a successful RYGB but stretched the Gastro jejunostomy join. This may be the most important cause of weight regain in bypass patients. The minimizer may play a vital role in preventing this. Also, leaving as little as possible bowel at the join is critical. This surgery is very difficult and requires a lot of thought before proceeding.